The Six-Million-Dollar Man and Bionic Woman may not be far off.
Like most service members who have lost limbs in Iraq or Afghanistan, 22-year-old Marine Corporal Christopher Santiago can instantly recite the exact time and surroundings when the IED exploded and destroyed both his legs.
He was in al Anbar Province in Iraq. It was 8 p.m. on 16 September 2006, near Saqliwiyah, some 15 kilometers west of Fallujah. His patrol was returning to base after a day of convoy duty, and Corporal Santiago, a tall, lanky youth from Parkersburg, West Virginia, had just gotten out of his Humvee to move some concertina wire that had strayed across the road inside the entrance to the Marine compound.
"I grabbed the wire with my left hand and took one or two steps over, and then—bam!—I was blown 10 feet or so and lying on my back," Corporal Santiago says, recounting the blast from a 130-millimeter improvised explosive device that was embedded in the dirt. "I was shocked because it was right on our base. I remember that when I was picking up the concertina wire, I was thanking God we had gotten through another patrol. After a second or two on the ground, I started checking my body with my right hand. I had no pinkie or ring finger on my left hand, and a five-inch bone was protruding from my arm. I couldn't move either leg or my left arm, and my right foot was severed, hanging by a thread. I raised my right hand and yelled, 'It's me—Santiago—over here! I need a corpsman.' "
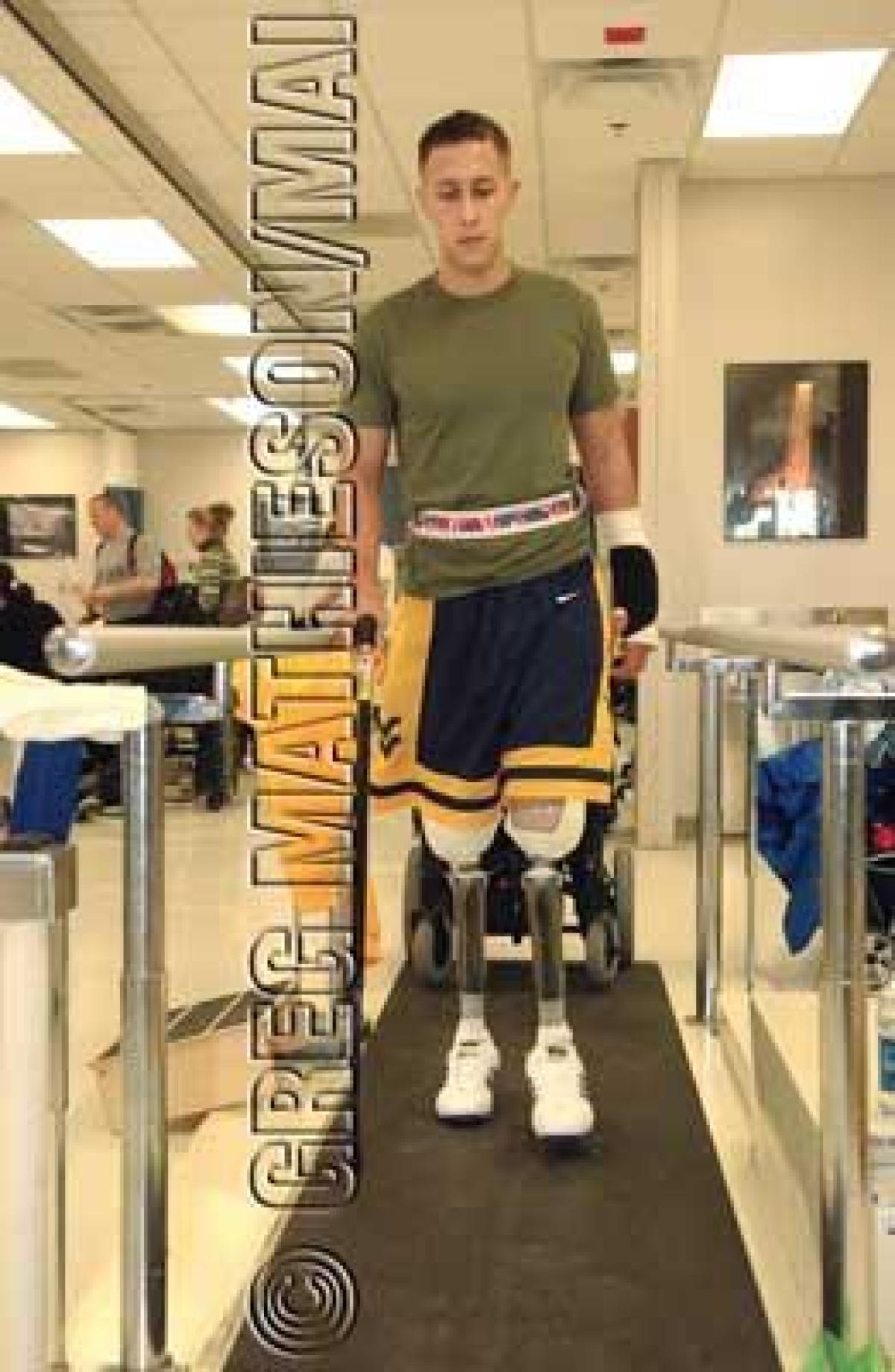
Ten weeks later, after the amputation of both legs in Iraq, and interim stops at the Army Regional Medical Center in Landstuhl, Germany, and the National Naval Medical Center in Bethesda, Maryland, Corporal Santiago was at Walter Reed Army Medical Center in Washington, taking his first steps on a pair of artificial legs. The $50,000-a-leg prostheses had been custom-fitted to what little remained of his legs—the residual limbs, as physicians call them. The prostheses are battery-powered "C-Legs," each equipped with a microprocessor that bends a mechanical knee when he shifts his body weight and adjusts automatically to his stride.
Along with an array of other factors, such high-tech prostheses have dramatically improved the treatment of service members such as Corporal Santiago who lost their limbs in Iraq or Afghanistan, compared to that available to wounded troops in previous conflicts. With wounds that would have been fatal during the Vietnam or Korean wars, today's GIs more often survive the trauma, then come home for surgery, weeks of therapy, and an electronically controlled prosthetic arm or leg.
From Sci-Fi to Reality
Moreover, military and civilian researchers are developing a new generation of computerized prosthetics—expected to be available in five to seven years—that promise to be as close to real limbs as those portrayed on such then-fanciful 1970s science-fiction shows as The Six-Million-Dollar Man or The Bionic Woman. On the drawing-boards are plans for artificial arms and legs that patients will be able to control by moving what remains of the same muscles (on their residual limbs) that they used previously to set their natural limbs in motion, or in some cases by merely thinking about what they'd like the prosthetics to do. Electrodes implanted into the peripheral nerves of their residual muscle—or imbedded in the brain—will sense the electrical impulses associated with the intended motion and use them to activate the prosthetic device. The same circuitry will enable those who lost limbs to tell whether their artificial arms or legs are positioned where they want them and to sense it when the arm encounters heat, cold, vibrations, or other conditions.
To be sure, it isn't just the technology that has improved the outlook for the grievously wounded. Combat medical corpsmen in all the services are much better trained and equipped these days than they were in Vietnam or Korea; many carry what amounts to a portable operating room in their packs so they can treat traumatic casualties right in the field. The military has developed far more effective procedures for evacuating the wounded and flying them to hospitals where the patients can be stabilized, increasing their survival rate. Medical techniques have advanced significantly. Today, service members are treated by teams of doctors—orthopedists, general surgeons, plastic surgeons, and neurosurgeons—who work together using advanced procedures for everything from skin grafts to muscle-flap repair.
Also important is that the returning troops enjoy visible support—from medical personnel, from their families, and from the public at large—that wasn't always there during the Korean and Vietnam conflicts, says Army Lieutenant Colonel Paul Pasquina, chief of physical medicine and rehabilitation at Walter Reed.
"The big difference is that the public has learned how to separate their political feelings from the love and respect for the troops who are doing the fighting," Colonel Pasquina says. "The community support is huge, and that far outweighs the advances in technology. It's not just saving lives—it's a continuum of care."
Indeed, at Walter Reed, the service members themselves serve as something of a 24-hour-a-day self-support group. No longer kept in bed for months, they get up into wheelchairs quickly and eat together, attend physical therapy sessions together, and keep each other's morale up. The hospital provides a wide range of professional services, from exercise training to counseling. A Defense Department program provides free housing and food to families so they can be with their loved ones for as long as they are hospitalized. Even recreational activities are geared toward helping patients build strength and gain confidence. The summit is a trip to Utah, during which recipients of artificial limbs can take a turn at skiing.
More and Younger Losses
The need for dramatic gains in treatment has become particularly acute over the past four years because proportionally more troops are coming home with limbs missing. There are several factors behind this trend. First, with improvised car and roadside bombs now so widespread in Afghanistan and Iraq, GIs are more likely to encounter explosions close-up. While body armor and Kevlar vests protect vital organs from bullets and shrapnel, arms and legs still are exposed—and often are blown away when the bombs go off. Meanwhile, battlefield medical treatment and evacuation techniques have improved, and the survival rate for the wounded has increased significantly. Ten percent now die of their wounds, compared to 30 percent in previous conflicts. But the proportion of wounded troops who end up losing arms or legs has doubled—to 6 percent, from 3 percent in past wars.
Defense Department figures show that since the U.S. invasion of Iraq in March 2003, more than 539 members of the Armed Forces have lost limbs as a result of their tours in Iraq and Afghanistan; 93 of these have lost more than one limb. More than three-quarters of the 539 have been treated at Walter Reed. Others go to the Brooke Army Medical Center in San Antonio, or to the National Naval Medical Center in Bethesda.
During much of the post-Vietnam War period, amputees—both at Walter Reed and at Department of Veterans Affairs (VA) hospitals around the country—tended to be elderly men with diabetes whose amputations became necessary as a result of the disease, medical officials say. By contrast, today's battlefield casualties are young, physically fit men and women who need—and expect—better medical results. Dozens missing limbs have asked to remain on active duty. Some even want to go back to back to Iraq. Corporal Santiago is planning on going to college after he leaves the Corps.
Compared to the technology available in previous conflicts, today's array of options for those who have lost limbs is impressive. Along with the C-Legs that Corporal Santiago uses is another robotic prosthetic called the Rheo Knee. Both use microprocessors that analyze the amputee's gait, based on the shift in his body weight when he walks, and adjust the speed and degree at which the mechanical knee bends. As a result, an amputee can alter the way he walks to fit the surface he's walking on—so that his gait and stride look normal.
"When I put on long pants, nobody notices," says Army Specialist Matthew Pennington, a 23-year-old artilleryman from Troy, Maine, who lost his left leg after a roadside bomb exploded and destroyed his Humvee during convoy duty just north of Tikrit last April. Specialist Pennington plans to run for town manager when he leaves the service.
Fine-Tuned Matching
Fitting such leg devices is a delicate and painstaking process. Technicians take a cast of the patient's residual limb and convert it into a mold for the prosthesis' socket cuff, which holds the artificial limb to the residual limb or body. They then attach the cuff to the prosthetic leg, a rod of carbon steel and titanium that's connected to a computerized robotic motor in the knee. While the basic sections of the leg are manufactured by commercial prosthesis-makers, Walter Reed maintains a workshop where prosthetics specialists fit the parts together, customize the cuff and leg for each patient, and program the computers and robotic motors.
In a special gait-and-motion analysis lab, technicians measure a patient's stride and gait by photographing his walk with special infrared cameras that track reflective markers taped on his body. An extra-sensitive scale measures the impact of the service member's body motion on torque. The results are analyzed and converted into a stick-figure computer image, and the package is sent to prosthetists and physical therapists. Less sophisticated videotapes are shown to each patient to help him—or her—change the way he walks so as to be able to use the leg more naturally.
Indeed, the results can be impressive. Not only are those who have lost limbs walking sooner and more effectively than they did a decade ago, but many are regaining skills that would challenge even those with real-life limbs. Many quickly learn to walk without a noticeable limp. And every day in Walter Reed's exercise room, patients fitted with prosthetic legs maintain an eye-popping pace on mechanical running machines. Soldiers who have lost a leg are qualifying for jump duty in the Airborne. One amputee treated at Walter Reed recently competed in the Iron Man Triathlon, an annual swimming-biking-running race in Hawaii.
Even so, the recovery process isn't easy. Corporal Santiago was unconscious for much of his travel from Iraq to the United States, spent several days in intensive care units in Landstuhl and Bethesda and underwent a series of skin- and tissue-grafts to his left hand. This month he'll have reconstructive surgery at Walter Reed to rebuild his left arm. To help increase his strength, he spends much of the day in the center's physical therapy room, walking between parallel support bars from 0800 to 1100 and exercising his arm and thigh muscles in the afternoon.
A Friday in mid-December was the first day he was able to use his C-Legs without a cane. "It was an amazing feeling—it really felt great," he said recently. But, he added, "I'd really like people to know how difficult all this really is."
Specialist Pennington's experience wasn't any easier. Besides losing his left leg, he suffered a massive loss of blood and extensive damage in his right leg. After a spate of transfusions at Landstuhl, he underwent 13 operations at Walter Reed, where physicians inserted rods, performed skin-, muscle-, and bone-grafts on his left arm and leg and reconfigured his remaining limb. He was fitted for a prosthetic knee and leg in June, but couldn't walk until the end of September.
"The hardest part is the bleeding at the end of the stump," he said. "It really hurts at first."
The Boundaries
What's more, even the current prosthetics technology has its limitations. The prostheses require a certain amount of bone around which to attach the socket cuff, often requiring a higher amputation than otherwise might be necessary. If the residual limb is small, the artificial leg can be heavy and uncomfortable, requiring a good deal of effort for the patient to move around. Although the socket cuffs are custom-made, the size and shape of a residual limb changes frequently during the day, sometimes leading to chafing and occasional infection. The limb can overheat, requiring hours of downtime for them to cool and recover. Often, more surgery is needed before a limb can be made to fit properly. Some of the wounded find it difficult to maintain their balance with a new prosthesis, and they sometimes fall, especially when they try to turn suddenly. In some prostheses, the knee locks instantly when the lithium battery that powers the mechanical knee runs down, leaving the leg temporarily unusable and sometimes bent at an awkward angle.
Today's technology for artificial arms is impressive, but less advanced than that for legs. Because arm, wrist, and hand movements are far more complex than knee/leg movements, it's more difficult to develop prosthetics that can perform the functions an amputee needs to regain some of his previous capabilities. Typically, artificial arms come with a hook-like pincer, or gripper, that enables the person to pick things up, along with an array of snap-on tools that let the patient work in the kitchen, write, cast a fishing rod, and even play golf. There's also a cosmetic snap-on that looks like a real hand but can't do much that's useful besides shaking hands and holding a glass. To move the arm in most prostheses, the patient must flex specific muscles located in the upper arm, shoulder, or neck, which exerts tension on a cable that's attached to the prosthesis. Other prostheses are controlled by electrical leads attached to the outer skin of the residual limb within the socket, where they can record small electrical signals from underlying muscle activity, which can be translated into arm or hand movements; the quality of such external signals is sketchy and is degraded when the electrodes slip or when the skin sweats or overheats.
The drawbacks in the current technology for upper-body prosthetics are more serious than that for legs. The prostheses for arms don't provide nearly the kinds of capabilities that the service member had before his limb loss, and the restrictions on how much weight the patient can pick up make all but light lifting impossible. Upper-limb prostheses also can be more difficult to use. Shifting your right shoulder to move your left arm is a counter-intuitive motion that's difficult to master and often seems unnatural, making the benefits of such prostheses seem not worth the hassle to some. The patient can rotate his wrist, but typically he can't flex it or extend it.
Additional Research
Nevertheless, science is coming to the rescue—and quickly. The Defense Advanced Research Projects Agency (DARPA), which shepherded the invention of the Internet before that technology was made available for civilian use, is spearheading a $50 million Manhattan Project-style program to develop next-generation arm, wrist, and hand prosthetics that promise to overcome the shortcomings of the current technology and dramatically improve the performance of upper-extremity prostheses.
Although the year-old crash effort won't be fully completed until 2010, researchers already have produced two beginning prototypes—unveiled this past December—that mark stunning improvements over today's upper-extremity prosthetics. Army Colonel Geoffrey Ling, the physician (and veteran of the conflict in Iraq) who serves as the program manager for the DARPA project, says they should be ready to submit for Food and Drug Administration approval within a year.
"Right now, if you look at the prosthetics for arms and hands, all they have at the end is a hook—just like Captain Hook in Peter Pan—and that's not enough," Colonel Ling says. "Our vision is to have a prosthetic arm that's controlled by the brain, and we're going to do it. It's going to be light-years better than what we're using now."
The new technology centers on developing prosthetics that tap signals from the primary motor cortex—the part of the brain that controls voluntary movement. When an amputee wants his arm or leg to move, the brain sends a signal to the central nervous system. A miniature computer translates that signal and sends it to a robotic prosthesis, which then moves as it has been ordered. The scientific journal Nature reported last summer that the technique has been used with some success in enabling paralyzed patients to control computer cursors—and to move objects using a robotic arm. Using such an implant, a 25-year-old man whose spinal cord had been severed learned to move objects simply by thinking he wanted to do so. Eventually, he learned to operate a television set, open e-mail, and pick up small objects with a robotic arm.
Microchips in Robotic Limbs
At the same time, researchers at the VA's Advanced Platform Technology Center of Excellence in Cleveland have been experimenting with a system that implants the electrodes in the remaining portion of a patient's arm or leg so the mechanism can sense the minute electrical activity that he makes when he intends to move his limb. Much like the one involving brain signals, the impulses are fed into a tiny microprocessor that controls a robotic limb. Scientists say the same kind of system can be used in reverse to give the patient the kind of sensory feedback he would receive from a living arm: the ability to sense touch, temperature, vibration, and position—that is, how far he has moved his arm and where it is now in relation to the rest of his body. The artificial limb would be stronger and better able to endure heat, cold, water, and humidity, and would change its shape and stiffness to correspond to the condition of the wearer's tissues.
"Developing prosthetics that have a direct connection to the nervous system is going to be a quantum leap in providing patients with far great capability," says Dr. Ronald J. Triolo, a biomedical engineer who is executive director of the Cleveland VA's Advanced Platform Technology Center. While such techniques are still in the developmental stage, they're apt to be ready for use by patients in five years, he says. "What we're trying to do here is to jump-start advances in materials, microelectronics, and neural interfaces and apply them to prosthetics."
Indeed, just this past month, researchers began human trials on a next-generation prototype arm developed at the Johns Hopkins University's Applied Physics Laboratory in Laurel, Maryland, which is coordinating one of the DARPA projects. The state-of-the-art device, unveiled in December, uses surface electrodes in combination with signals from remaining nerve fibers in the patient's residual limb to control a mechanical arm system that permits seven different arm, wrist, and hand motions instead of the three that most current prostheses can carry out, and also gives the patient better control of coordinated motions. Although the artificial fingers move as a unit, they bend in conjunction with a movable thumb, for the first time enabling a user to pick up a suitcase, for example, and to flex and rotate his hand.
And scientists at the DEKA Research and Development Corporation, the Manchester, New Hampshire, firm that invented the Segway personal transporter and an all-terrain, stair-climbing wheelchair, unveiled a separate prototype in December in which the prosthetic is controlled by nerve impulses from the brain that have been moved to the patient's chest and hooked up to electrodes. The device also enables the user to receive sensory feedback that gives him a light sensation when the arm encounters pressure.
continue reading...
Play the Piano?
Stuart Harshbarger, the biomedical engineer at Johns Hopkins who heads the four-year DARPA program that taps the work of dozens of government agencies and private universities, calls the breakthrough just a taste of what is to come. In a three-phase effort, the consortium plans to build two even more advanced prototypes between now and 2009 that will provide patients with up to 27 different finger, hand, wrist, elbow, and arm motions, controlled by tiny electronic sensor circuits that can be injected into the peripheral nerves of a residual limb. Future prototypes also will send wireless signals to a signal-processing module in the socket of the prosthesis to control the limb's mechanical movements.
Mr. Harshbarger says if the experiments are successful, the incremental improvements pioneered in the prototypes now in the works should be available at Walter Reed and other treatment centers—for limited use at first—in as little as one to five years, along with feedback mechanisms that enable the user to sense when the arm encounters heat, cold, vibration, and other changes. And DARPA's Colonel Ling says his agency has been working closely with the FDA in an effort to speed approval of the new prosthetics when the testing has been completed.
"Our long-term goal is to develop a prosthetic arm whose hand can grasp and throw a baseball, play the piano, or pick up a flower and place it in a vase as naturally as a biological arm"—all tasks that are too difficult for the current generation of prosthetic limbs—Mr. Harshbarger says. "I want to be realistic about what the public can expect," he says, cautiously. But, he concedes, the gains so far have stunned even the scientists who are working on the project. "It's really kind of hard to believe," he exclaims.
Although the various new approaches reflect years of research and development, the field is still in its infancy, and there are myriad obstacles to overcome. As the research papers published in Nature admit, the current system using brain signals requires that the patient be tethered to a bulky cart of equipment, and the equipment needs constant fine-tuning. The prototype implant has wires that penetrate the skull and skin, but it has a high risk of infection. Friction from implants can lead to neuro-scarring.
Yet scientists say the advances promise to be breathtaking. The best prosthetic hands in use today rely mainly on a single open-and-close pincer and can lift only about nine kilograms of weight. By contrast, those being developed will contain 22 or more joints, will be able to lift between 22 kilograms and 27 kilograms and will bend more fully, enabling the wearer to manipulate objects that are fragile, such as eggs. In some models, the computer will be able to guess what the patient's neurons are trying to accomplish, and re-configure the hand to accomplish them. To top that off, the prosthetic will have a mechanical frame and will be coated in flesh-colored silicon to make it resemble a real arm or hand.
The Remaining Challenges
The new techniques also would eliminate many of the problems that the current generation of prostheses poses, says Troy Turner, portfolio manager for the prosthetics research effort at the Army's Telemedicine and Advanced Technology Research Center at Fort Detrick, Maryland. Users no longer would have to master a system for controlling their limb movements by flexing a shoulder or thigh muscle, which can be confusing and difficult. The devices would be less prone to infection or damage from dust, weather, and extreme temperatures. And battery power would be more reliable than it is now.
Scientists say the major remaining challenges in development of the new technology are centered on two areas—how to make sense of the various signals that are generated by neurons, and how to design computer chips that can interpret them rapidly enough to make the whole system usable.
Yet there's little doubt that the technological breakthroughs are coming soon. Improvements in prosthetics are being unveiled and made available to hospitals and clinics almost constantly. And public interest in such developments—particularly for use by veterans—is increasing. In a 2004 book called The Long Way Home, cartoonist Garry Trudeau shows the trials faced by his "Doonesbury" character B.D. as he recuperates from a leg loss suffered after a rocket-propelled grenade attack near Fallujah. The volume, which includes 84 separate episodes, is laden with details about prosthetics and rehabilitation. Taken by the plight of those who have lost limbs, Trudeau has been visiting injured vets himself.
Michael Weisskopf, a Time magazine war correspondent whose right hand was blown off in Iraq when he tried to toss away an explosive device that was thrown into the Humvee in which he was riding, has written a book, Blood Brothers: Among the Soldiers of Ward 57, published last October, which describes his own struggles and those of three others who were in the same vehicle and survived. He, too, continues to visit the wounded at Walter Reed.
Meanwhile, Corporal Santiago remains undaunted. "When I got off all the initial narcotics, the realization about what had really happened set in," he recalls. "It was sad, but there was nothing I could do about it." He's not sitting still, however. He plans to apply to West Virginia University and major in business and economics.
"I'm not sure yet whether I want to go to graduate school," he says. "For the moment, my biggest goal is just to walk."
Mr. Pine, a former naval officer, is a veteran journalist who has worked as a Washington correspondent for the Baltimore Sun, Washington Post, Wall Street Journal, and Los Angeles Times. He was Proceedings' 2006 Co-Author of the Year.
Mr. Mathieson is an internationally acclaimed photographer best known for his work for NBC News in Iraq.